Not every lump or bump that you feel in your breast is cancer, so lets talk about some of the more common mimickers of breast cancer that just might freak you out!

Regardless of your age, we encourage all of our patients to examine their breasts at least once every month. Why? Well, did you know that most breast issues, cancer and non-cancer alike, are actually discovered by people examining their own breasts? It makes sense when you consider the fact that no one knows your breasts better than you do and the more you examine them, the better you will know them.

When doing these BSE’s (Breast Self Exams), you will likely find lumps, bumps and other changes that might concern you. Luckily, most things that you find during a BSE will actually not be breast cancer, so to put your mind at ease, here are some of the more common conditions of the breast that will likely freak you out but are not cancer.
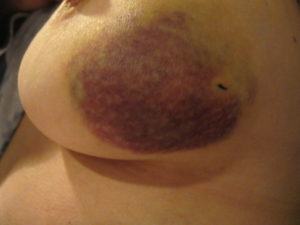
Fat Necrosis: The majority of the breast is made up of fat tissue and Fat Necrosis is a condition that occurs when some of that fat becomes injured. This injury can be from something as simple as an unintentional blow to the breast or it can occur after a medical procedure like a biopsy or breast surgery. The damaged fat tissue actually dies off (tissue death is called necrosis), forming a painless lump filled with liquefied fat. The skin over the lump may be red and bruised and dimpling of the skin and retraction of the nipple may also be present.
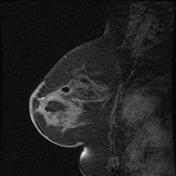
Fat Necrosis: Diagnosis is usually made by a combination of history, clinical breast exam, imaging like mammography and ultrasound and frequently a needle biopsy to remove the fatty fluid. Fat Necrosis does not require treatment and does not increase your risk of breast cancer in the future.
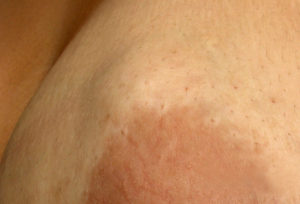
Fibroadenoma: Fibroadeomas are fairly common, with up to 5% of women being diagnosed with one at some point in their lives. Fibroadenomas are not malignant (cancer) but having one does slightly increase your risk of developing breast cancer in the future if it is not removed. Fibroadenomas are firm, rubbery, circular and mobile. These benign tumors occur most often in women in their 20’s and 30’s and if untreated they may get larger over time. Diagnosis is by clinical breast exam, imaging like mammogram or ultrasound and biopsy to ensure no underlying cancer is present.
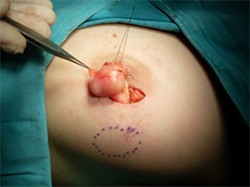
Fibroadenoma: Fibroadenomas do not have to be treated surgically but if they continue to grow, they should be removed both for cosmetic reasons and to rule out underlying cancer.
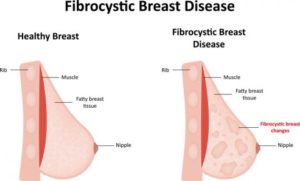
Fibrocystic Breast Changes: Fibrocystic Changes of the Breast are probably the most common change that we notice when examining a patient’s breasts. In fact, up to 50% of women actually have fibrocystic changes which are caused by a thickening of the normal breast tissue combined with small, fluid filled cysts. Women with Fibrocystic breast changes may notice small, tender nodules throughout both breasts, increased breast tenderness especially in the upper, outer portions of the breast, as well as increased tenderness and breast enlargement during the week leading up to the menstrual period.
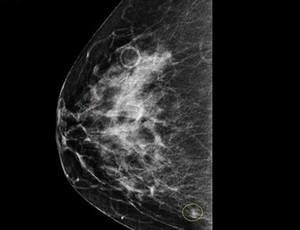
Fibrocystic Breast Changes: Your doctor will generally be able to tell you if you have Fibrocystic changes just by examining your breasts but definitive diagnosis usually requires imaging (mammogram or ultrasound) and sometimes a biopsy. Fibrocystic changes do not increase your risk of breast cancer and they do not require treatment. If you are experiencing pain and swelling some options include: 1). Heat or ice to the breasts, 2). anti-inflammatories like NSAIDs, 3). wearing a well fitted bra, 4). reduced touching and stimulation, 5). salt reduction to reduce total body swelling, 6). diuretics to reduce total body swelling and 7). hormonal therapy like birth control pills. Evening Primrose Oil and Vitamin E have also been found to reduce breast inflammation and pain.
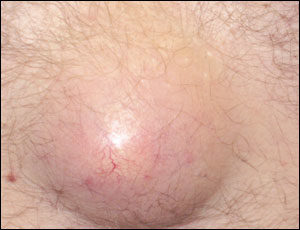
Lipomas: Lipomas are more commonly seen in women over the age of 40 and they are simply collections of fat walled off by a thin capsule. Lipomas are soft, mobile and generally painless. You doctor will initially do a clinical breast exam followed by some type of imaging, either an ultrasound or a mammogram. Biopsy may sometimes be recommended, but usually imaging is sufficient and will be repeated in a few months to make sure that nothing changes. If a lipoma is growing or you just want it removed, surgical excision is a possibility.
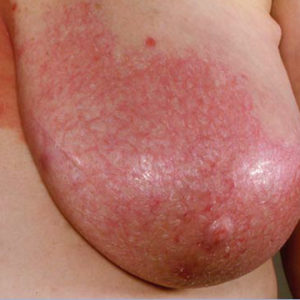
Mastitis: Mastitis is an infection and inflammation of the breast tissue. Mastitis is usually seen in women who are breastfeeding but it can also occur in non-breastfeeding women. Symptoms of mastitis include breast redness and inflammation, breast pain, fevers, chills and fatigue. Mastitis associated with breastfeeding is diagnosed with both clinical breast exam and usually an ultrasound to make sure that an underlying abscess is not present. Non-lactational mastitis usually requires a mammogram and potentially a biopsy to rule out an underlying cancer. Treatment usually includes continued breastfeeding (for lactational mastitis), rest, pain relievers and antibiotics.
While there are a ton of things that can mimic breast cancer, you should always be hypervigilant for the possibility of actual breast cancer. Make sure that you do your monthly BSE (Breast Self Exam), have a yearly clinical breast exam by your doctor and have breast imaging (usually mammogram) when recommended, usually starting at the age of 40. Signs of breast cancer can include:
- A palpable lump that is firm, irregular and does not move.
- Breast redness and/or inflammation.
- Skin dimpling.
- Nipple retraction.
- Enlarged lymph nodes under the arm pits.
If you didn’t catch Dr. J and I on The Ed Lover Show talking about breast cancer, you can check it out right HERE

 December 10, 2017
December 10, 2017





 May 19, 2018
May 19, 2018 



